Honest, paywall-free news is rare. Please support our boldly independent journalism with a donation of any size.
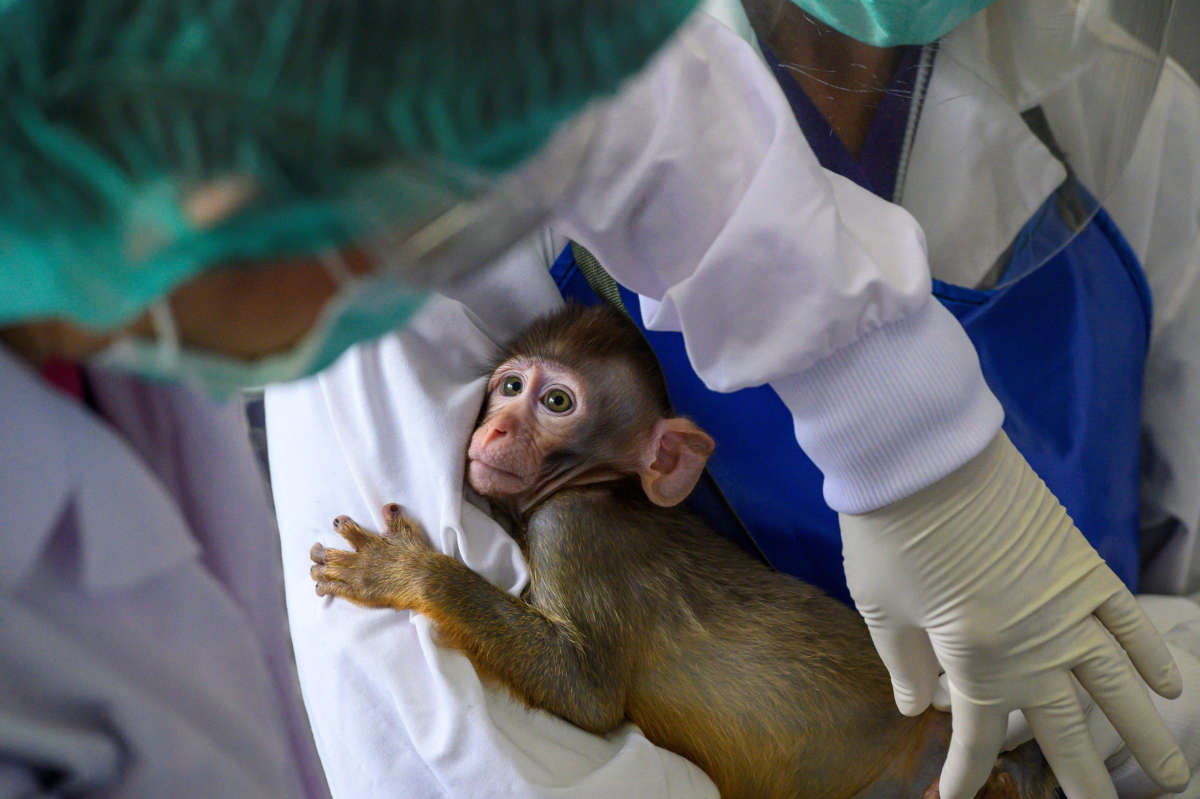
There have been concerted efforts on the part of primate researchers to convince the public and political leaders that more money and monkeys are needed for COVID-19 vaccine research. It’s not surprising that monkey researchers would attempt to exploit people’s fears about the pandemic to increase “supplies” and funding for their work.
What is surprising, however, is the complete lack of differing scientific views offered. The problem with the assertions made by pro-monkey research groups is their lack of supporting evidence.
Most findings in animals, including nonhuman primates (NHPs), do not predict human results — and, thus, far from being helpful, they are actually misleading.
More than 700 human trials of potential HIV/AIDS vaccines have been conducted, all of which gave encouraging results in animals including monkeys and chimpanzees — yet not one has worked in humans. In fact, some HIV vaccines actually increase the risk of HIV in humans. And as models of human diseases, NHPs have failed for Alzheimer’s and Parkinson’s diseases, neuroscience/brain research, stroke, cancer, hepatitis C, and many more.
More than 90 percent of drugs that appear to be safe and effective in animals fail in human trials. Vaccine development has an even higher failure rate. Only 6 percent of vaccines make it to the market. Can you imagine if you boarded a plane, and the pilot announced that you have a 6 percent chance of landing safely at your destination? You would demand an overhaul of the entire airline industry. Yet, when it comes to the safety and effectiveness of the vaccines and drugs we put into our bodies, monkey researchers want you to believe that clinging to the tools of old (i.e., monkeys) is a good idea. We don’t see anyone suggesting we should stick to the 8-track tape when we can stream music on our phones.
There is a valid reason why we need diverse representation in human clinical trials. No one human can accurately represent how a vaccine or drug will work in another human. How can we expect another species to effectively predict biological responses in humans?
Although COVID vaccines were tested in animals for regulatory reasons — tradition-based, rather than science-based — there is devil in the detail. Biologically, very different processes are occurring with the COVID-19 virus. Mice proved difficult to infect with the virus, even when genetically modified to make them more susceptible. If they did show symptoms, they were mild. Different species of monkeys also failed to replicate human symptoms, and where symptoms did appear, they too tended to be mild, reflecting different infectious processes.
Human trials of the Oxford/AstraZeneca vaccine proceeded despite prior monkey data that showed it did not prevent infection, and the Moderna vaccine was first encountered by humans without preceding animal trials. This would not have happened if the animal trials had been a crucial step in ensuring safety and efficacy.
Expert opinion agrees: the chief medical officer at Moderna stated, “I don’t think proving this in an animal model is on the critical path to getting this to a clinical trial.” Operation Warp Speed’s chief scientific adviser said Human data is “100 times more significant” than NHP data, and Anthony Fauci stated that translating animal vaccine results to humans has been “one of the banes of our existence.” Pfizer and BioNTech recognized early on that mRNA vaccines work very differently in animals compared to humans.
Biomedical research is increasingly utilizing innovative techniques that are human-specific. These techniques include human mini-organs (organoids) and human organs-on-a-chip, where 3D cultures of human cells are housed on small chips, with circulatory systems and other means of mimicking real-life function and physiology of actual human organs and the human body.
These techniques are being used ever more widely in disease research and in drug discovery and development, and were used in pivotal stages of the COVID-19 vaccine development, alongside computational approaches to their design. Entire human immune systems can be cultured, as can lymph nodes (pivotal to immune function) specific to individual people to reflect interhuman variability, and reflective of both diseased and healthy states — all without the confounding issues of extrapolation between different species.
For the sake of human health, our tax dollars should be directed into the best science. Whichever way you look at it, future biomedical research, including vaccine development for pandemics like COVID-19, will be based on human biology and human-specific testing methods. These methods are quicker, cheaper, more humane and — most importantly — relevant.
An urgent fundraising appeal: 48 Hours to raise $22,000
Thank you for reading Truthout today. We have a brief message before you go —
Unfortunately, donations are down for Truthout at a time when media is under immense pressure. Trump is arresting journalists, Big Tech is censoring independent news, and economic conditions for media have been worsening for years.
Simultaneously, movement media is vital in the fight against Trump’s authoritarian reign. Our mandate to tell the truth, share strategies for resistance, and speak against fascism is ever more urgent in this deluge of political censorship. Yet, we are struggling to meet our publishing costs when our work is so urgently needed.
If you can support Truthout with a one-time or monthly donation, you will make a significant impact on our work. Please give today during our fundraiser (only 48 hours left).