Truthout is a vital news source and a living history of political struggle. If you think our work is valuable, support us with a donation of any size.
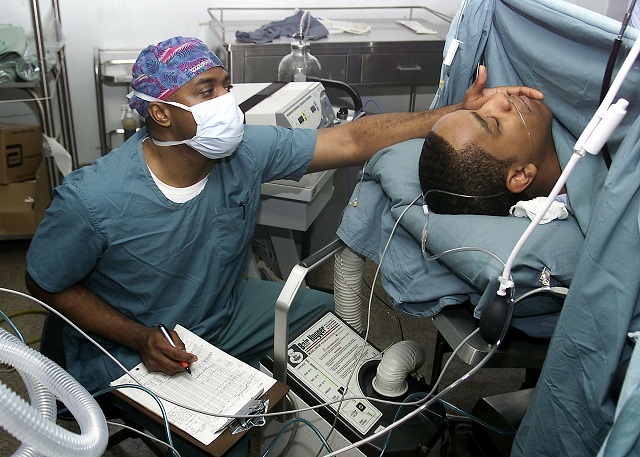
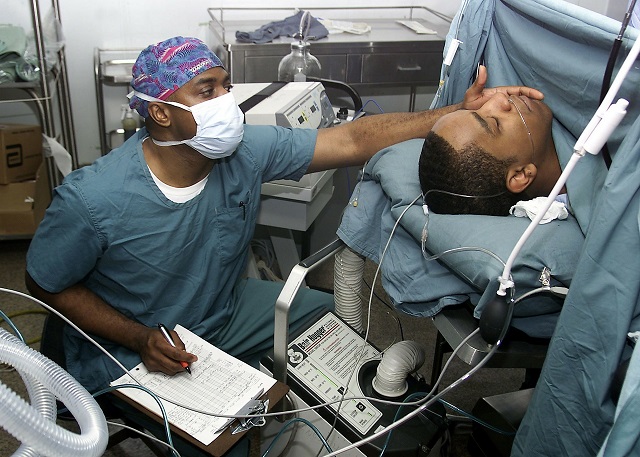 Studies have confirmed bias exists in health care — expressed as discrimination, prejudice, stereotyping and uncertainty. However, training can result in better communication and consequently, better outcomes for patients. (Photo: Pixabay)
Studies have confirmed bias exists in health care — expressed as discrimination, prejudice, stereotyping and uncertainty. However, training can result in better communication and consequently, better outcomes for patients. (Photo: Pixabay)
In problem-solving, groups benefit from the creativity that comes from diverse viewpoints. In medicine, the consequences of a lack of diversity are life and death. Diversity of thought has been associated with better decision-making in science, medical care and educational pedagogy.
As a transplant psychiatrist for the past 25 years in a multidisciplinary medical team of transplant surgeons, transplant hepatologists, and nephrologists, cardiologists, nurses, social workers and professionals in other specialties, I directly see these benefits.
That is because transplant is the ultimate teamwork endeavor. The liver transplant selection committee, for example, determines patient candidacy for liver transplant. The liver is a scarce organ, meaning more liver organs are needed than are available. According to the United Network for Organ Sharing, 20 people die each day desperately waiting on transplant lists.
The team occasionally ventures into difficult, contentious discussions about medical suitability for listing. We engage in vigorous debates regarding social, psychological and ethical issues in a patient’s candidacy.
Discussions may turn to evaluating personal patient attributes, such as the will to live, quality of family support, potential compliance with medications or medical care after transplant, and more. The more the discussions stray from data-driven analysis, the more potential there is for human bias to enter the deliberations.
Each team member needs to be aware of his or her own bias. A seminal 2002 National Academy of Medicine study shows that individual physician bias, described as discrimination biases and prejudice, stereotyping and uncertainty was linked to unequal treatment.
In other research, Lisa Cooper at Johns Hopkins University reports in her studies that race similarity between patients and physicians can improve some of the doctor/patient communications with African-American patients.
Studies using the well-established Implicit Bias Test (IAT) have shown that medical students and physicians have unconscious implicit biases for or against groups including African Americans, obese individuals and disabled patients. The upside of knowing your unconscious biases is that you can work to override them with knowledge, mindfulness, feedback and the time or space to reflect.
Usually everyone on the transplant selection team has an opinion and potentially everyone is deadly wrong. This is where the diversity of the people in the room matters.
The individual team member’s life experiences of adversity and resilience, racial and cultural sensitivities, and people’s courage to disagree and openly express the minority opinion, is crucial for a thoroughly considered, wise decision.
For the most part, the outcome is a sage decision by the teams comprised of individuals from different professional backgrounds, training programs and heuristic points of view. To work, a respectful and trusting stance toward others with whom you may disagree is crucial. In the end, it takes more than specialty diversity to successfully navigate the challenges to good transplant care and uphold the awesome responsibility of properly stewarding scarce organs.
Groupthink by physicians with a common knowledge base and sense of purpose may translate into easy consensus and collegiality. However, the lack of diversity in groupthink can also result in a lack of respect for patients.
So it is with medical “dark humor” or gallows humor, as it’s described by Katie Watson, an assistant professor at the Center for Bioethics and Medical Humanities at the Feinberg School of Medicine at Northwestern University. Watson writes that these seemingly harmless jokes may decrease anxiety in stressful health care settings, such as emergency rooms and transplant selection committees, but these jokes have consequences.
Such dark humor was part of a recent news story inspired by the comments of Peter Muennig of Columbia University and Alex Green of Massachusetts General Hospital. Hurtful words can potentially influence health care delivery.
Another 2016 study analyzed non-Black physicians’ words and suggest that non-Black physicians with higher implicit racial bias use more words reflecting social dominance and anxiety with Black patients.
Clearly, the medical profession needs to address these issues.
As a diversity dean at the Feinberg School of Medicine at Northwestern University for the past 15 years, my work ensures that diversity and inclusion is integrated into medical education and patient care.
Diversity is recognized by the Association of American Medical Colleges as a driver of academic excellence. Medical schools work to field a diverse group of talented students from different geographic, socioeconomic, racial and narrative backgrounds. This has led to some increase in representation of the under-represented in medicine groups over the past 20 years.
But results have been disappointing.
A 2017 study using the IAT showed significant white preferences among admission committee members. However, the study also shows that committee members’ knowledge of their IAT test results had a positive effect on their subsequent behavior. Despite the same number of underrepresented in medicine (URM) acceptances, a more diverse class result the next year suggests that something in the admission process was perceived more favorable by URM students.
Medical schools have also been challenged to improve and evolve medical school curriculums to better root out implicit bias during training. Through intergroup discussions and structured programs such as Sustained Dialogue, medical students can engage in difficult conversations and hot topics, so hopefully, when faced with dissentient viewpoints in practice, they’ll be more mindful to challenge their own assumptions.
The ultimate goal of all this soul-searching is to serve people with diverse needs effectively and to maximize health care outcomes. In real life, the best decisions come from a diverse group of thinkers.
Press freedom is under attack
As Trump cracks down on political speech, independent media is increasingly necessary.
Truthout produces reporting you won’t see in the mainstream: journalism from the frontlines of global conflict, interviews with grassroots movement leaders, high-quality legal analysis and more.
Our work is possible thanks to reader support. Help Truthout catalyze change and social justice — make a tax-deductible monthly or one-time donation today.