
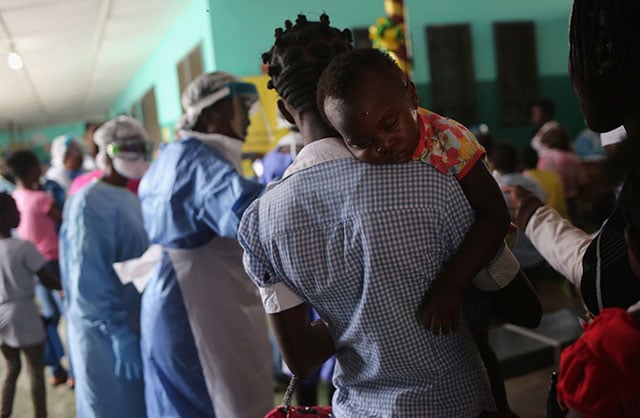
 People await treatment in the outpatient lounge of Redemption Hospital, formerly an Ebola holding center, on February 2, 2015, in Monrovia, Liberia. Many Americans suffer from the same lack of access to facilities and affordable drugs as patients in Liberia — yet the US spends more on health care than any other country in the world. (Photo: John Moore / Getty Images)
People await treatment in the outpatient lounge of Redemption Hospital, formerly an Ebola holding center, on February 2, 2015, in Monrovia, Liberia. Many Americans suffer from the same lack of access to facilities and affordable drugs as patients in Liberia — yet the US spends more on health care than any other country in the world. (Photo: John Moore / Getty Images)
The US Congressional Budget Office has confirmed what many of us suspected: The bill proposed by Sen. Bernie Sanders to allow Americans to buy prescription drugs from Canada and other countries would save US taxpayers $6.8 billion over 10 years. When Sanders introduced the legislation, he pointed to the absurd disparity between what Americans shell out for prescription drugs compared to the amount paid by people in other countries: $1,112 per person in 2014, compared to $772 in Canada and $325 in Denmark.
The US health care system is often found lacking when compared with those found in wealthy Western European countries. But how does the US system compare with poorer countries, such as Guinea or Liberia? It turns out that much like people in Africa’s poorest communities, many Americans suffer from both lack of access to facilities and exorbitant drug pricing. The main difference is that the US spends more on health care than any other country in the world.
For rural people in Liberia and Guinea, the distance to the nearest health care facility can mean the difference between life and death. In 2014, the Ebola outbreak in West Africa devastated both countries largely because of paltry health care infrastructure. Public and private actors already active in these two countries were forced to step in. In Liberia, the charity Last Mile Health, which trains people from remote villages to serve as community health workers, ramped up its efforts to help communities spot and stop the spread of Ebola. They accelerated their work at the clinic level, distributing essential equipment and teaching health workers how to deal with the virus in areas where it can take two days to walk to the nearest doctor.
In remote parts of Guinea, the epicenter of the outbreak, the Russian aluminum company UC RUSAL was one of the few entities with resources on the ground. RUSAL stepped in to build treatment facilities, bridging the gaps in the official network of health care facilities. The Centre for Epidemic and Microbiological Research and Treatment, built by the company in 2015 as part of a public-private partnership with the Guinean government, accelerated diagnosis, research and treatment delivery. That investment has already proved critical in bolstering Guinea’s fledgling anti-epidemic efforts.
In the US as well, difficulty of access is a persistent, pernicious problem. In a recent survey of patient accessibility, when US respondents were asked if they could get a same- or next-day appointment with their provider, 52 percent said no. One challenge is human resources: for all the money it spends, the US has fewer general practitioners per capita than most developed countries. The problem is worse in rural areas, where those who live far away from the one or two doctors in town miss out on vital care. The Affordable Care Act (ACA) may have attempted to address the insurance barrier to health care, but it couldn’t solve issues like doctors not being present in certain areas.
Neither did the ACA solve the inherent contradictions of a system in which receiving treatment depends on whether or not you have private insurance. Hundreds of thousands of low-income patients in places like Eunice, Louisiana, still depend on clinics run by Americares and other charitable initiatives for screenings, medications and vital treatments. Americares sums up the reality of the situation with this disturbing quote from a community member in Eunice: “If it wasn’t for the clinic, they’d have to bury us in the backyard. There’s no way we could afford health care.”
The gaping holes in coverage produce spectacles like the Remote Area Medical Expedition, a charity event held at a county fairground in rural Virginia last month. The idea comes straight out of the volunteer medical missions that help critically underserved communities throughout Africa, Latin America and Asia. As it turns out, Americans are just as much in need. The “Expedition” Virginia stop drew more than 2,000 people who still struggle to afford co-payments and prescription drugs in the wealthiest country in the world.
Ideally speaking, the world’s richest country would be able to treat and prevent diseases while improving patient access to care. Here too, though, the US continually fails to provide affordable medicine. Patients at the Virginia pop-up medical camp included diabetics who can’t afford insulin injections. Insulin, as one of the volunteering doctors pointed out to the New York Times, has been on the market for nearly a century.
Many African patients have the same problem, though at least they can point to moving in the right direction thanks to the rapid growth of local pharmaceutical industries. Countries like Swaziland have been making impressive strides in providing lower-priced drugs. Thanks in part to financial support from the US’s President’s Emergency Plan for AIDS Relief (PEPFAR) and the Global Fund to Fight AIDS, Tuberculosis and Malaria, 171,266 HIV-infected people in Swaziland now receive antiretroviral drugs (ARVs). That has driven down HIV incidence from one of the highest levels in the world to 1.4 percent. This 44 percent decrease would have been impossible without affordable drugs.
In the US, on the other hand, pharmaceutical companies continue to vastly overcharge consumers. Martin Shkreli, who infamously hiked the price for a critical AIDS drug by over 5,000 percent, is just the poster child for price gouging. In Louisiana, 35,000 residents with hepatitis C are on Medicaid or uninsured, but treatment costs $85,000 for a 12-week regimen. The company behind the treatment, Gilead Sciences, charges $55,000 in Canada and only $33,000 in France.
The state of the US health care system is galling. The campaign to repeal Obamacare was just one step backward; immigration restrictions on the foreign doctors who fulfill critical needs in remote areas, along with plans to cut funding for medical research, seem like unfathomable self-inflicted wounds. Unfortunately, Trump’s impact doesn’t stop at US shores: His announced budget plans would also reduce contributions to PEPFAR, one of the most successful anti-AIDS programs in history, by 17 percent to $3.8 billion. Not content with gutting his own country’s health care system, Trump apparently wants to jeopardize lives in Swaziland as well.
Join us in defending the truth before it’s too late
The future of independent journalism is uncertain, and the consequences of losing it are too grave to ignore. To ensure Truthout remains safe, strong, and free, we need to raise $27,000 in the next 24 hours. Every dollar raised goes directly toward the costs of producing news you can trust.
Please give what you can — because by supporting us with a tax-deductible donation, you’re not just preserving a source of news, you’re helping to safeguard what’s left of our democracy.