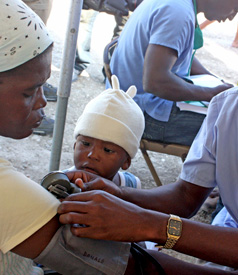
Alternative Health Care in Haiti, Part IV
With the motto “Providing a preferential option for the poor in health care,” Partners in Health offers an unusual model of health care provision. Its mission is both medical and moral.
Partners in Health is widely recognized as changing the potential for health for low-income people and countries throughout the world. Partners in Health’s extraordinary success comes from its philosophies regarding health and justice, which include a belief in the power and dignity of the patient; a commitment to health care as a human right; and an understanding that true health for the poor can only come through challenging the poverty which causes so much illness. The success of the group also comes from the zeal with which it pursues its philosophies through hands-on medical and social care in several countries.
In a rare interview, Loune Viaud tells about Partners in Health’s Haiti program, Zanmi Lasante, or Friends of Health. Loune serves as Director of Operations and part of the strategy and planning team in Haiti.
Beverly Bell: Tell us about Partners in Health, how it constitutes an alternative in health care, and especially how its philosophy has contributed to bringing about another model of care in Haiti.
Loune Viaud: We started in Haiti more than 25 years ago. We realized right away that you can’t talk about health without talking about the social aspects of health: justice and rights. That’s why we try to embrace a lot of social elements underlying health. When a patient is sick, we don’t see the sick person only, we see the environment and community they came from. After they leave the hospital and go back home, will they have water to drink? Do they have a place to live? Do they have food to eat? Can they send their children to school? Do they have work? We try to touch on all of it: job, home, nutrition, malnutrition, agriculture. We try to touch on schooling and sanitation, meaning potable water.
That’s why we don’t just consider ourselves a health organization, although we have a big medical team: doctors, nurses, pharmacists, lab technicians, etc. We also have community health workers, outreach agents, and agricultural agents who live in the communities and strengthen those communities.
BB: We know that Partners in Health’s work is not only a social program, that it’s tied to the idea of transformation, to the idea that as long as people are living with injustice and inequality they won’t enjoy good health. I understand that people that in the village of Cange, where Partners in Health has been for so many years, really trust the group, and that this is one of the reasons you’ve have better success with people following HIV/AIDS treatment programs than even the National Institute for Health. How is power connected to the issues of treatment and the relationship to the patient?
LV: I don’t want to start rejoicing about what you call success because we still have a lot of work to do. It’s forward, forward, forward. Matter of fact, every time we see the numbers going down, we make more efforts to see if we can get them to zero.
I can’t say that we change the lives of the people completely, but we’ve seen improvement.
Let’s take, for instance, an HIV patient. We know that if that person can’t afford medicine, can’t eat, can’t send their kids to school, doesn’t feel that they’re heard as a person and seen only as a patient, that person’s not going to get well. But when people are sick and know that they can count on an organization to help them send their children to school, then they can concentrate on improving their lives, which means taking their medications. When people are sick and know they don’t have to keep on drinking the river water they used to drink but can drink potable water instead, when they don’t have to live in a straw hut in poor sanitary conditions and get bitten by mosquitoes anymore… even though physically they’re not totally well, morally they know that they’re recognized as a human being.
I think what makes us successful is our accompaniment program. Take tuberculosis, a disease of poverty. When a person comes in and tests positively for tuberculosis, what we do is send an accompanier to visit that person’s home to see the social conditions they’re living in. If that person sees they need a new house, we work with the community to get them a house that, as we say, can’t fool the rain. In terms of water, we set up filters or other catchment and treatment systems. The accompanier goes to visit the sick person each day, assures that the patient takes their medications, assures that if the patient has a problem that he or she listens. Even if the accompanier can’t solve the problem, the very fact that the person can talk about it and someone can listen without judging is really important.
Well, at that point, if the accompanier can’t solve the problems by him or herself, he or she will go talk to the supervisor in the hospital. The accompanier becomes an advocate for the sick.
Health also goes alongside education. Early on we realized that the best thing we can do in a community is to send children and the youth to school so that they don’t spend their time in the streets. What we did, starting in Cange, was to create a school with trained teachers, books, and at least one hot meal for the kids so they can concentrate and study. The parents don’t have to worry about where they’ll find money to pay. Now we have 15 schools throughout the Plateau Central. We have thousands of students, children who go to study, sometimes just primary school if that’s what the town has, though in Cange the school goes up to 12th grade.
We also send young people to study in universities in Cuba and the Dominican Republic, or we send them to study nursing in [the Haitian towns of] Léogane and Gonaives. We help them find scholarships to go to Europe for specialized studies.
BB: From the perspective of Partners in Health, what do Haitians need to be a people with good health?
LV: Access. One of the things that really frustrates me and makes me mad is to find someone who’s walked eight or ten hours to get to our hospital in Cange, sometimes in terrible pain. For that person to go through what it takes to get there, you can imagine how advanced the sickness must be. Sometimes it’s almost too late. If that person could stay where they lived, they could go to the clinic or the dispensary early on, without having to go far from the community.
That’s what people need: access to care. But I’m not just talking about access through proximity. It’s not just about building a hospital or a health clinic nearby and then asking people to pay. If the care or the medication is expensive, the people won’t get it.
It’s access, access, access. It’s the right of people to heath care when they need it, drinking water, sanitation. If you offer these things that are far away or that people can’t pay for, it doesn’t serve them. They have the right to have their needs met, quantitatively and qualitatively.
BB: So does that mean that everything that Partners in Health does is free of charge?
LV: I always avoid saying that our services are free. Health care is expensive. Someone pays. But not the poor, because they can’t afford it. We don’t want the poor to pay with the little that they have. We don’t want them to say, “I don’t have money, so I’m not going to the doctor.” We don’t ever want that to happen.
People pay with what they have. Sometimes they carry on their heads bananas, fruits they grow, they bring a chicken, you understand. They bring what they can so that they can pay. But we always struggle that it’s not the poor who pays for the care.
BB: If we’re looking at structural change, we know that at the end of the day it can’t be done through NGOs, in Haiti or anywhere else. NGOs can’t replace the state. But all of us who know Haiti know that right now the state isn’t fulfilling or can’t fulfill its responsibility. Are you doing advocacy vis-à-vis the state to make it assume its responsibility to the citizens, now or in the future?
LV: The state is the one who’s in place, legally, to respond to the needs of the people. What Partners in Health tries to do is to collaborate with the state so that if there’s weakness in one aspect, we can reinforce its efforts, so that down the road it can better meet its responsibility.
Do you like this? Click here to get Truthout stories sent to your inbox every day – free.
We always say that the Ministry of Health is our most important partner. We realized a long time ago that it doesn’t make sense for us to do our own little efforts apart, to build our own hospital or clinic or even separate schools. We insure that everything we do supports and reinforces the Ministry of Public Health, the Ministry of Education, and the Ministry of Agriculture. If there were a Ministry of Housing or Water, we’d support them, too. We don’t invest in separate efforts.
Apart from [Partners in Health’s hospital in] Cange, we work with ten public hospitals. We started supporting the Ministry of Health in these hospitals in 2002. And then, we’ve started building what’s going to be one of Haiti’s best hospitals, in Mirebalais. It will have a training program for residents in a partnership with national medical school. That’s twelve hospitals where we’re working, in all.
For the most part, we’re strengthening the state-run hospitals. But when you take, for instance, the hospitals in [the towns of] St. Nicolas and St. Marc, really Partners in Health provides a lot of staff. We pay for salaries and equipment. We’re really part of managing the hospital with the Ministry.
BB: Please tell us about what’s happened since January 12th. Partners in Health has played an important role after the earthquake, assuring that at least some people have received the care that they need.
LV: January 12th came upon us without warning. We started clinics in four [internally displaced people’s] camps. We have almost 400 employees – doctors, nurses, lab technicians, pharmacy technicians – that we’ve hired since January 12th to provide medical services in these camps.
One of the first things we did after the earthquake was to start supporting the government in the largest hospital, the University Hospital [also known as the General Hospital]. We provided and coordinated volunteers; we came with medications and equipment that they needed. There are fewer and fewer volunteers coming now, but our work continues so people can get the care they need in a hospital, with dignity.
We haven’t signed anything officially with the Ministry of Public Health. It’s really an engagement with the directors of the University Hospital to support the place. We’re not managing it. It falls into our line of work to support what the Ministry is doing.
Also, with other partners we’re creating a foundation, Friends of the University Hospital, to really rebuild the hospital and make it into what it should be. We’re working with the national medical school, too, so students can get training there.
BB: If I understand correctly, Loune, you weren’t trained in health care or management. You came to help at Partners in Health and you got your “doctorate” on the job.
LV: I’ve been at Partners in Health for 22 years. When you start working here, you enter a vocation. You have to love it to do it because it doesn’t pay very much. You do it because you truly believe in the human being. We at Partners in Health treat every person as though it were our own sister, brother, mother, child.
BB: I’m guessing you have a great need of funding.
LV: Like I said, this work is expensive. We’re always looking for people to help pay so the poor don’t have to. We’re looking for partners, as our name implies – as long as they share the philosophy and understand what we’re trying to do. Alone we can’t do this work. It’s the work of many hands. If you look at our logo, it’s hands together.
To support Partners in Health’s work in Haiti, please go here.
Join us in defending the truth before it’s too late
The future of independent journalism is uncertain, and the consequences of losing it are too grave to ignore. To ensure Truthout remains safe, strong, and free, we need to raise $34,000 in the next 72 hours. Every dollar raised goes directly toward the costs of producing news you can trust.
Please give what you can — because by supporting us with a tax-deductible donation, you’re not just preserving a source of news, you’re helping to safeguard what’s left of our democracy.